Get 40 Hours Free Developer Trial
Behavioral health teams are already dealing with enough complexity. They need a system that reduces friction across intake, documentation, scheduling, billing, or follow-up care. That is a big reason behavioral health software is getting more attention from organizations that have outgrown generic healthcare systems.
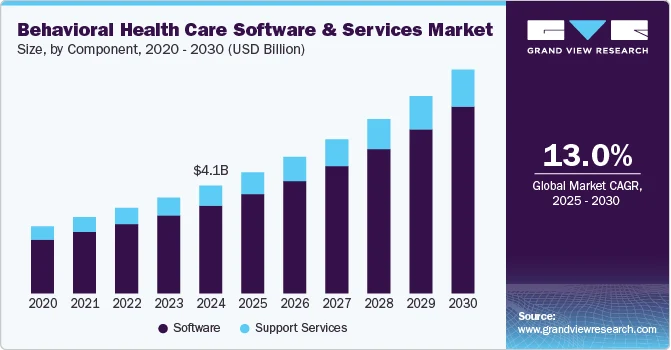
This shift is not only about digitizing operations. It is about giving clinicians, coordinators, and admin teams workflows that actually reflect how behavioral care works in the real world. Grand View Research estimates the global market was $4.14 billion in 2024 and projects it to reach about $8.61 billion by 2030.
Developing these systems involves different software requirements than a common healthtech system. The platform needs to handle extended patient treatment periods while enabling complex record keeping, protecting sensitive information, and running its daily business activities.
What is Custom Behavioral Health Software?
Developing custom behavioral health software creates a system that mirrors the real operational flow of everyday behavioral health treatment. The system creates a customized solution for therapy practices, psychiatric services, substance use programs, and integrated care teams who require different combinations of documentation, scheduling, billing, care coordination, and patient engagement functions.
Behavioral health treatment requires extended time periods of care, which results in more extensive documentation needs, multiple treatment sessions, continuous patient progress measurement, and stronger protection for private information. This customized system focuses on creating practical workflows that doctors and nurses need to perform their daily clinical duties through treatment plans, assessments, teletherapy, and role-based access and compliance controls.
Let’s design a system that supports your care model, compliance needs, and long-term growth. Start Your Project with Us.
Why Healthcare Organizations Build and Need This?
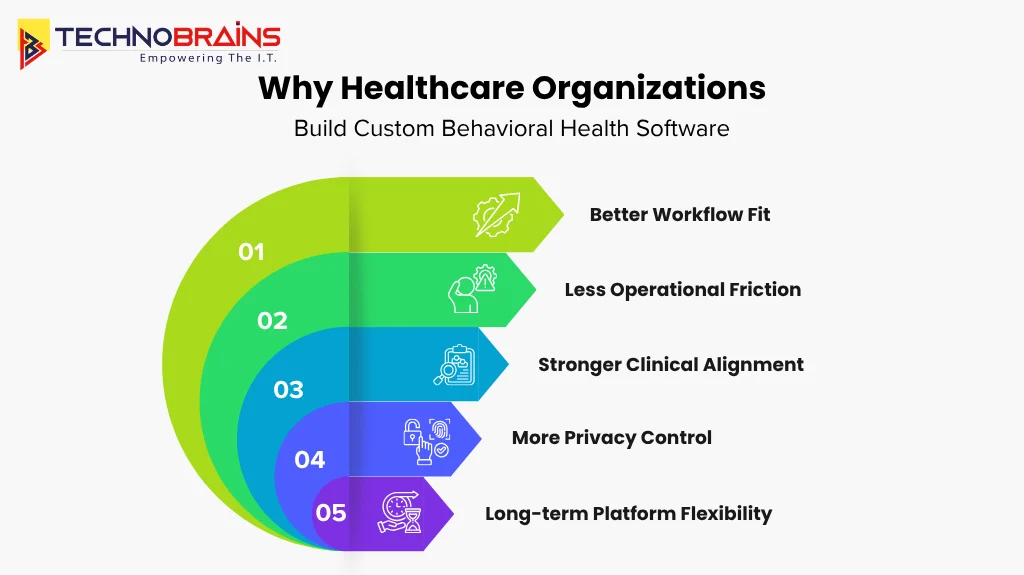
- Better workflow fit: The software is designed according to actual operational requirements, which need to handle recurring sessions, record detailed notes, create treatment plans, and manage long-term patient monitoring.
- Less operational friction: Many organizations today depend on separate systems to handle intake and scheduling, documentation, billing, and reporting tasks. Custom platform helps bring those workflows into one system.
- Stronger clinical support: Effective software enables clinicians to conduct assessments, coordinate care, monitor progress, and deliver teletherapy services through their customized workflows.
- More control over privacy and compliance: Modern systems require stronger access control systems, together with consent management tools and audit visibility features, because they handle sensitive treatment information.
- Long-term flexibility: Custom software allows organizations to manage their integration needs, reporting functions, and product development path, while standard vendor roadmaps restrict their control over these key areas.
Behavioral Healthcare Software vs General Mental Health EHR
A general mental health EHR supports records, scheduling, and basic billing. Custom behavioral health system goes further by supporting care delivery, operations, compliance, reporting, and integration needs across the organization.
| General Mental Health EHR | Custom Behavioral Health Software | |
|---|---|---|
| Primary focus | Clinical records, scheduling, and basic billing | End-to-end workflows across care delivery, operations, compliance, and reporting |
| Clinical documentation | Standard note templates and patient records | Therapy, psychiatry, SUD, and program-specific workflows with more tailored documentation |
| Care model support | Usually works for individual-provider or basic clinic setups | Better suited for integrated care, multi-program teams, group therapy, and long-term care coordination |
| Privacy and compliance | Covers standard healthcare privacy needs | Built with stronger segmentation, consent controls, and auditability for sensitive behavioral health data |
| Integrations | Often limited to standard EHR and billing needs | More flexible for telehealth, reporting, outcomes tracking, billing, and external healthcare systems |
| Customization | Usually configurable within vendor limits | Built around the organization’s actual workflows, roles, and operational model |
| Long-term fit | Works well for basic or early-stage needs | Better for organizations with complex operations, scaling plans, or specialized requirements |
Common Features of Custom Behavioral Health Software
The most effective software works according to the team’s daily operational needs, which is used to provide patient treatment, document their work, and operate their business activities.

Smart intake
A digital intake process should create a unified workflow for processing forms together with insurance information, consent documentation, and initial assessment procedures. This system minimizes front-desk duties while providing essential information to clinicians before they start patient care.
Session scheduling
Behavioral care often depends on recurring visits, reminders, cancellations, waitlists, and attendance tracking. A strong behavioral healthtech system should handle these as one connected scheduling workflow instead of scattered admin tasks.
Clinical notes
The platform should support narrative notes, treatment plans, assessments, and progress tracking without forcing providers into rigid templates. This is a key part because documentation in behavioral care is ongoing and detail-heavy.
Billing workflows
Completed sessions should connect smoothly to coding, claims, authorizations, denials, and payment tracking. In behavioral health, billing works best when documentation and reimbursement workflows are closely connected from the start.
Privacy controls
From the very beginning, the system needs to integrate access control and consent handling, audit trails, and sensitive-data segmentation. The project requires HIPAA-compliant software because it handles extremely confidential medical treatment information.
Struggling with disconnected systems and workflow gaps? Build a unified behavioral health platform designed around real clinical operations.
👉 Get a Custom Solution Plan!
Compliance Requirements for Behavioral Healthcare Software
In the system design process, compliance requirements must be included from the very beginning. The platform must protect patient privacy while managing therapy records, psychiatric care data, and substance use treatment information because these elements should not be treated as secondary.
HIPAA safeguards
HIPAA requires three types of safeguards that protect health information through administrative, physical, and technical security measures. The platform requires built-in security features, which include secure authentication, encryption, access controls, and audit logging to ensure protection from unauthorized access.
Part 2 controls
If the platform supports substance use treatment, the 42 CFR Part 2 regulation becomes more important. These rules place stricter limits on how certain SUD records are accessed, used, and disclosed.
Consent and auditability
Consent management, data segmentation, and audit trails should be part of the core workflow. The system should clearly show who accessed a record, when it happened, and whether that access matched the right permissions.
Secure interoperability
Behavioral health systems also need to exchange data securely with other platforms. That makes standards-based interoperability important, especially when providers, payers, and partner systems need cleaner data sharing.
Built-in compliance
The goal is not just HIPAA-compliant behavioral health software on paper. It is a system where privacy, security, consent, and auditability are built into the way the platform works.
Interoperability and EHR Integration
Interoperability is a key foundation for modern healthtech systems, which need to connect with Electronic Health Records, billing software, telehealth applications, laboratory systems, and reporting platforms. The presence of separate systems creates problems that result in double work, incomplete patient information, and delays in both clinical and operational processes. That’s why the necessity for HL7 integration occurs, because organizations consider it an essential element instead of treating it as a supplement to existing functions.
The goal is to achieve secure system connections that enable them to share information through safe methods that create usable data. Organizations need to establish their integration plans from the beginning, and they should implement standards-based exchange methods whenever they can.
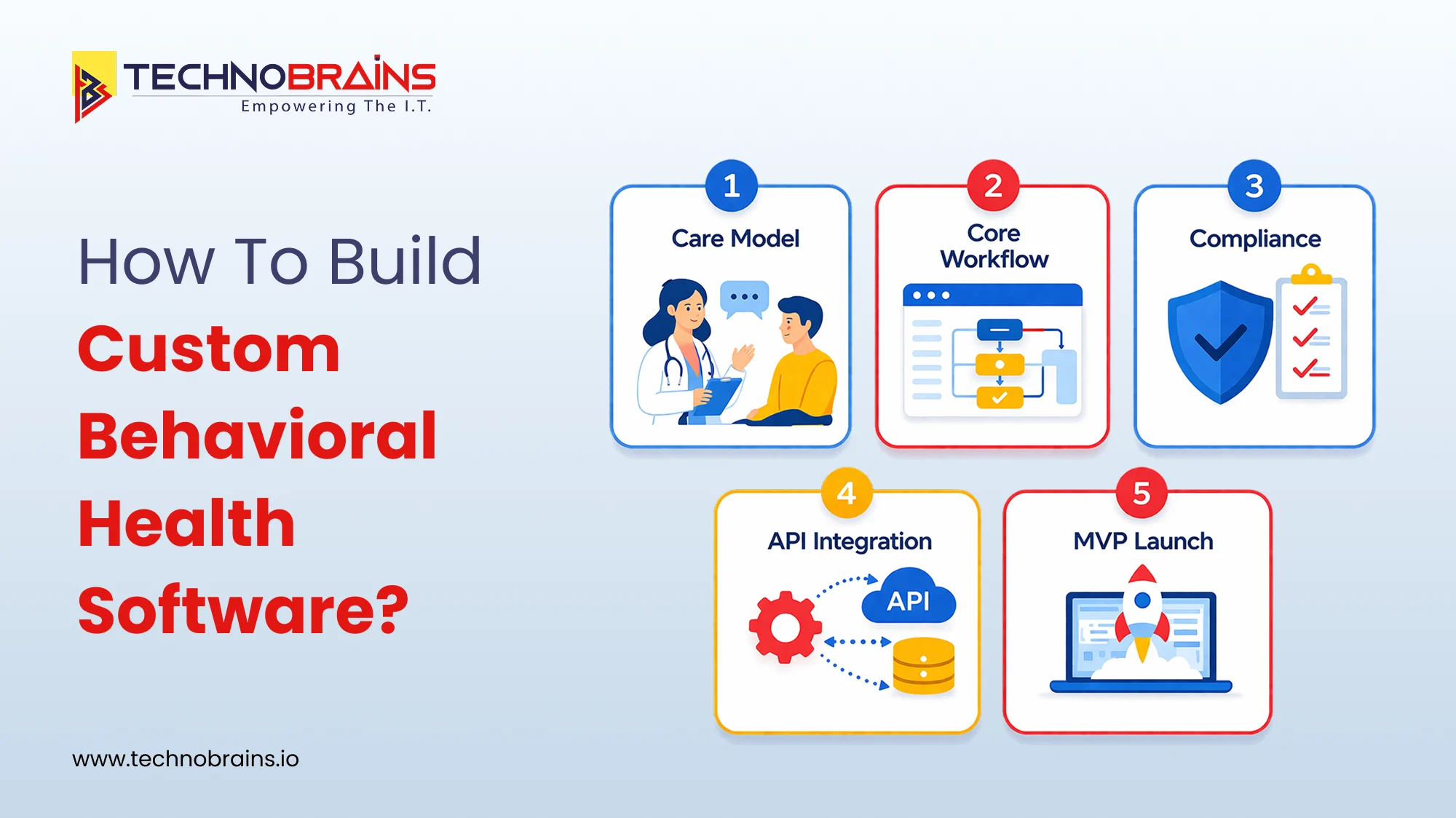
How to Build Custom Behavioral Health Software Step by Step
A custom healthtech system requires more than just determining which features to include. The implementation of operational procedures, regulatory standards, and system connection choices needs to occur during the initial development phase to prevent future schedule setbacks.
1. Define the care model
When developing the platform, you must determine its target audience and the methods by which you will provide care to them. Different types of therapy require different workflows, documentation methods, and privacy requirements for their operations.
2. Map core workflows
Before moving forward, you need to identify all essential elements of intake and scheduling, clinical notes, treatment plans, billing, consent handling, and follow-up care. The development process reaches its turning point at this stage, which determines whether they become effective systems or remain disconnected systems.
3. Set compliance early
At the start of the project, it’s important to implement privacy measures and access controls, audit systems, and compliance regulations. It starts with fundamental design decisions that remain unchanged until the final development stage.
4. Plan integrations upfront
From the beginning, determine how the platform will connect with EHRs and billing systems, telehealth tools, labs, and reporting platforms. The software implementation process benefits from strong integration planning because it minimizes unnecessary work while ensuring the program matches authentic clinical workflows.
5. Build the MVP first
Start by focusing on your core modules, which your teams require for daily operations, before expanding through subsequent phases. The majority of organizations require implementing intake and scheduling, documentation, assessments, billing, and privacy controls before they can proceed to advanced processes.
6. Test with real users
During pre-launch testing, organizations should include clinicians, administrative staff, and billing personnel in their evaluation process. The system has to deliver user-friendly systems for better adoption rates, operational effectiveness, and better delivery of healthcare services.
Cost and Timeline for Behavioral HealthTech Software
The cost and timeline for behavioral health software typically depend on workflow scope, compliance requirements, integrations, and rollout complexity. A focused MVP takes less time and budget, while a broader platform with EHR connectivity and billing, telehealth, reporting, and stricter privacy controls requires a larger investment.
| Build Scope | Typical Timeline | Typical Cost Range | What It Includes |
|---|---|---|---|
| MVP platform | 3–5 months | $60,000–$150,000 | Intake, scheduling, notes, assessments, basic billing, privacy controls |
| Mid-level platform | 5–8 months | $150,000–$300,000 | Telehealth, reporting, role-based access, and stronger workflow customization |
| Advanced platform | 8–12+ months | $300,000+ | EHR integrations, claims workflows, multi-location support, advanced compliance, analytics |
Common Challenges in Behavioral Health System Development
Workflow complexity: Behavioral health systems operate through multiple workflows because their various components, which include therapy and psychiatry, substance use treatment and care coordination, and billing and administrative operations, need platform support from their initial development stage.
Compliance demands: Privacy rules, consent handling, audit trails, and 42 CFR Part 2 requirements create multiple challenges that teams typically fail to recognize as essential parts of their work.
Integration issues: Connecting EHR systems with billing tools, laboratory systems, and reporting systems, and scheduling software proves more complicated than it appears during the initial planning stage.
Adoption problems: Platform needs to involve clinicians, administrators, and billing staff from the beginning stage because this practice helps with product adoption. The project requires special attention because it connects with a telehealth app, which needs a user-friendly design for effective usage.
Scope creep: One common issue in the first release occurs when developers attempt to deliver an excessive amount of content. The system should begin with essential workflows that will operate after going live under this more efficient method.
From our perspective, the right system is the one your team actually wants to use.
If you’re planning to build one, we can help you get it right from day one.
👉 Connect with Our Team!
How Technobrains Helps Build Custom Behavioral Health Software
Building the right behavioral health platform is not just about development capacity. It requires a clear understanding of behavioral clinical workflows, compliance requirements, integration planning, and the daily realities of care teams. That is where TechnoBrains helps organizations move from early planning to a platform that is actually practical to use.
We design and build custom healthcare software around the workflows that matter most, including intake, scheduling, documentation, billing, and privacy controls. The goal is simple: create a platform that aligns with how behavioral health teams actually deliver care, not force them to adapt to rigid systems.
Frequently Asked Questions: Behavioral Healthcare Software Development
It makes sense when the organization needs to use specialized workflows and handle sensitive information while operating multiple programs that need to connect with other systems.
Typically, most teams start with the core workflows they use every day, which include intake, scheduling, documentation, assessments, billing, privacy controls, and reporting.
Because the platform must establish privacy protections and user consent mechanisms, audit trail capabilities, and access control measures from its initial design.
Integration is especially important because various systems require patient information to transfer data between them while avoiding additional manual tasks.
The duration of the project depends on project scope and compliance requirements, and the degree of integration needed.